by Daniel Andrews | October 26, 2023

An image of a futuristic brain. Credit: Drug Target Review
What is Alzheimer’s Disease?
Alzheimer’s is a devastating form of dementia that affects 6.5 million Americans, and 55 million people worldwide. The disease is the seventh-leading cause of death and one of the primary causes of disability in elderly people according to the World Health Organization.
According to the Alzheimer’s association, it affects memory, thinking, and behavior. The symptoms, which include, but are not limited to, memory loss of new information, poor judgment, confusion, and changes in mood eventually grow prevalent enough to interfere with the completion of daily tasks. In the late stages of the disease, the loss of brain function (commonly causing an inability to swallow) results in dehydration, malnutrition, infection, and, ultimately, death.
Alzheimer’s is an incredibly devastating disease to both the victims and their loved ones. As someone whose family has been affected by Alzheimer’s, the results of the disease are tragic and make the patient highly difficult to care for. Millions of families slowly see their loved ones lose touch with themselves and the world around them, not to mention the economic and lifestyle challenges that accompany the treatment.
At the moment, there is no known cure for the disease, but some first strides have been made recently in the scientific community that have shown some promise towards one day finding a cure. In understanding how the drug works, it is first important to understand the basic neurological malfunctions that take place in the development and advancement of Alzheimer’s disease.
What’s going on in the brain of an Alzheimer’s patient?
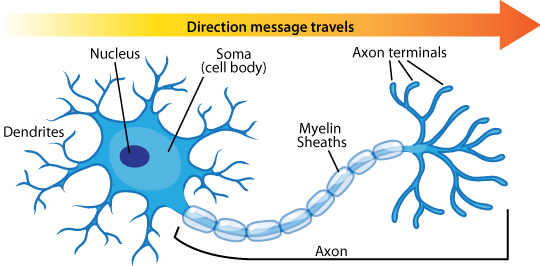
A diagram of a neuron that shows the cell body (soma), which contains the nucleus, with short branches (the dendrites) extending from it. Also, extending from the soma is a long tail (the axon), covered in myelin sheaths and branching out at the end into axon terminals. Credit: Arizona State University
There exists in the brain billions of neurons, which, according to the National Institute on Aging, are cells in the nervous system that relay messages throughout the body. In essence, anytime we move, have a thought, absorb information from the environment, or anything else, neurological pathways are being used. Each neuron has dendrites (these accept messages from other neurons), axons (which transmit messages), and the cell body (this has the nucleus with the cell’s DNA and regulates the neuron).
For those with Alzheimer’s, these neurological pathways get disrupted by something called amyloid plaque. This is a type of protein that occurs naturally in the brain but forms in excess over time in Alzheimer’s patients. The plaque grows and spreads between neurons, disrupting cell function and prevents them from communicating, regenerating, and metabolizing. As more cells die and plaque growth continues to spread, the brain becomes more and more damaged and the severity of the disease steadily worsens.
There are many other factors at play that cause Alzheimer’s, but the new drug that has been developed focuses on the removal of this amyloid plaque.
New drug shows promise
On July 7, 2023, the FDA granted approval for the first ever drug shown to clearly and effectively slow the progression of Alzheimer’s disease. The drug, called Leqembi, works by removing amyloid plaque in between neurons. According to the Washington Post, the drug slows cognititve decline by 27% over 18 months compared to a placebo. This is the equivalent to a 5 month delay in the disease’s progression.
This, while not a cure, is great news for Alzheimer’s patients and their families. It could mean they have another six months to drive or time to see their grandchild’s graduation. It’s also a promising stepping stone to possibly finding a cure some day. Science builds upon itself, and while it’s no guarantee, Leqembi offers a glimpse of hope that maybe this is the first step towards a cure.
Despite this encouraging news, it comes with plenty of downsides. For starters, the drug is only for patients in the early stages of the disease. Those with advanced Alzheimer’s will not benefit from the drug. The drug also requires transfusions with a needle twice a month, and possible side effects such as brain swelling.
The drug also costs $26,500 for a year’s worth of treatment. This, coupled with the possible side effects and modest efficacy, has sparked some controversy and skepticism. We have to remember, however, to tamper our expectations. While this is not a cure, it still has massive potential to improve the lives of patients and give way to future discoveries.
Alzheimer’s risk reduction
In the meantime, actions can be taken (or not taken) for you or your loved ones to reduce your risk of getting Alzheimer’s disease. Physical exercise is one of the most important things you can do to improve brain health. It increases blood flow to the brain and improves the health of blood vessels, both of which are imperative for a healthy functioning brain. Also related to blood circulation is smoking, which has been shown to disrupt blood flow and therefore increase your risk of Alzheimer’s in addition to other health problems. Excessive alcohol intake should also be avoided, as it can lead to brain degeneration and damage.
If possible, it’s also best to follow a mediterranean diet. Foods such as leafy greens, certain fruits, and fish rich in omega 3 fatty acids have all been shown to improve brain health and memory among other health benefits. Getting enough sleep is also crucial in promoting brain health and aids in the clearance of amyloid plaque in the brain.
How can Frenalytics help?
With Frenalytic’s innovative personalized cognitive recovery program, patients’ therapy evolves around personal images and experiences to help them regain functionality.
Frenalytic’s patented auto-collection and progress monitoring data analysis allows clinicians to track their progress in real time, while sharing the data with loved ones.
Like it or not, Alzheimer’s is still affecting millions of people around the globe, and these people need help now. Frenalytics is there with Alzheimer’s patients, step by step, until one day a cure is hopefully found. Until then, our personalized learning plans help you or your loved one stay standing despite the devastating blow of Alzheimer’s.
Engage Your Mind with Frenalytics™ – signup for a free trial, or call (516) 399-7170 to learn more.
Want to see how Frenalytics helps patients and students live more independent lives?
Click here to create a free account, or give us a call at (516) 399-7170.
Dan Andrews is a Junior at Boston College studying Finance and Philosophy. His time at Frenalytics has helped him gain a clearer insight into the needs of persons with disabilities and the importance of an effective learning process. Dan enjoys skiing, hiking, reading, and spending time with his friends and family. Contact Dan: dan@frenalytics.com

